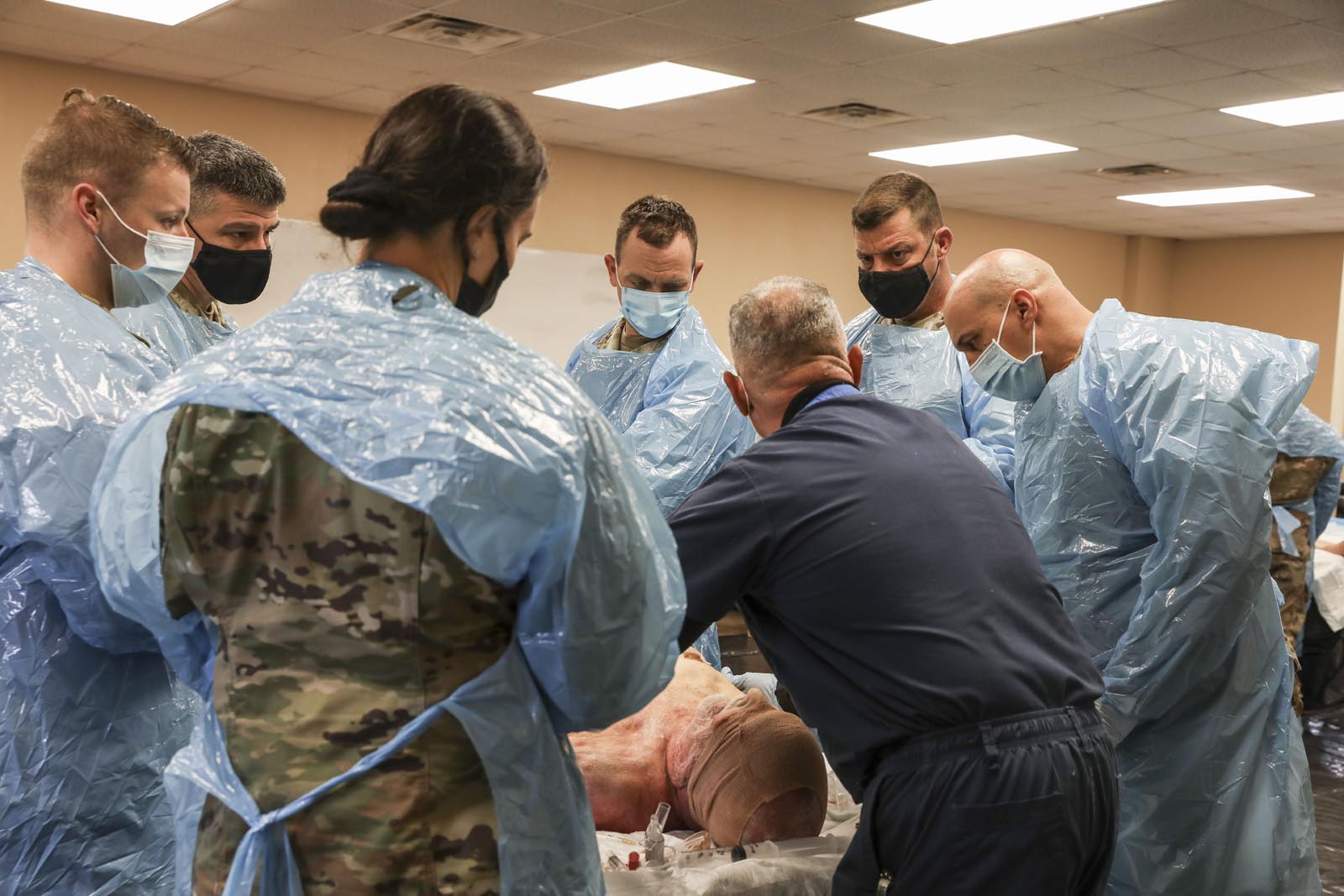
First National Guard program to host medical cadaver training on NG post
By Staff Sgt. Noshoba Davis, Louisiana National Guard Public Affairs Office
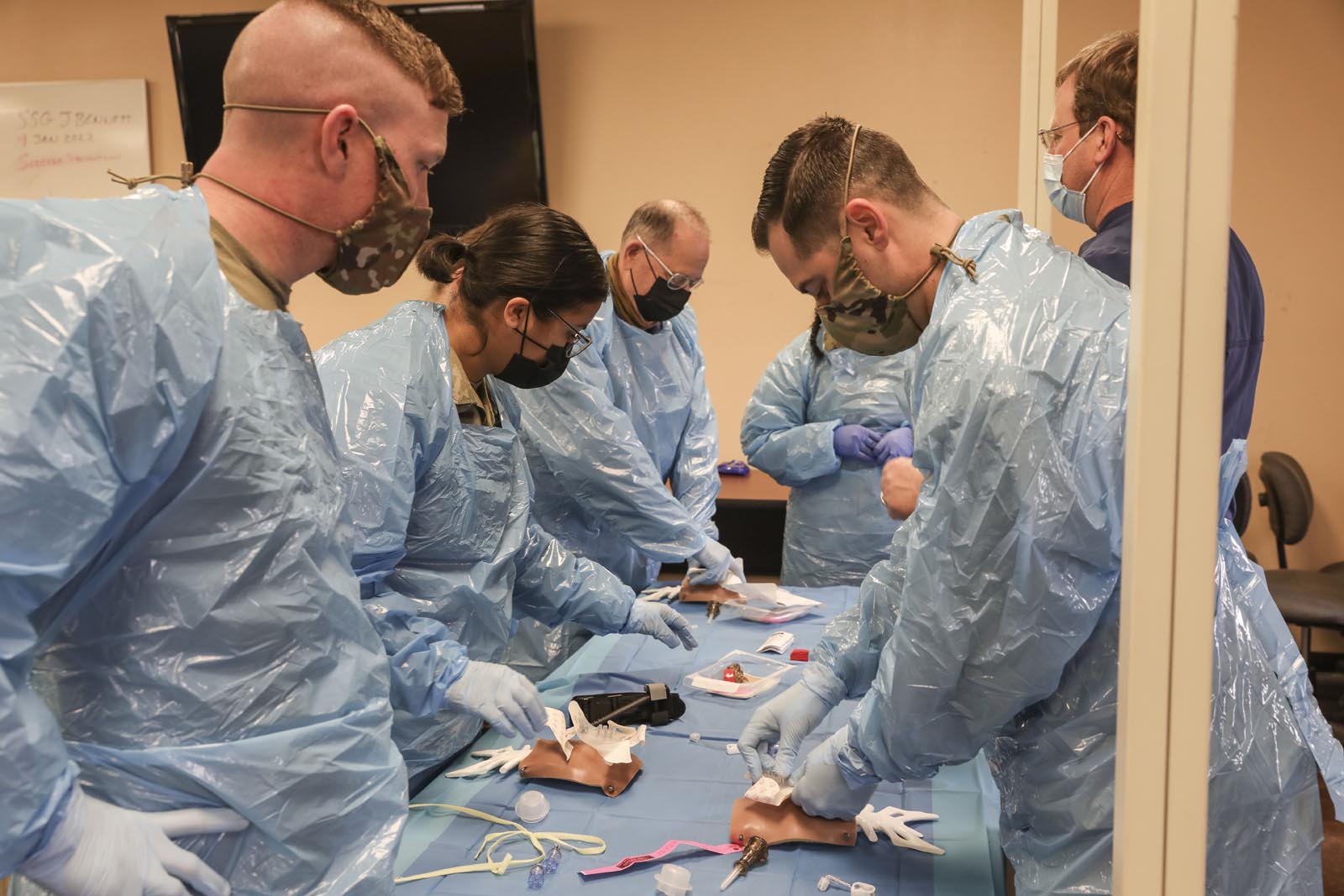
PINEVILLE, La. – The Louisiana National Guard’s combat medic (68W) sustainment program recently held a cadaver training lab for combat medics and medical personnel at Camp Beauregard in Pineville, Jan. 21.
Sgt. 1st Class Howard Bushey, the combat medic sustainment program director, arranged to add the cadaver training lab to the beginning of the LANG’s medical sustainment training. The lab was coordinated through the LANG’s State Surgeon’s office, Teleflex Medical Equipment and Medical Education & Research Institute (MERI).
This is the first time Teleflex and MERI have conducted the training on a National Guard post. The training, open to all components wanting to participate, hosted more than 100 soldiers and airmen from the LANG, Regular Army and Reserve components.
“I think that when you’re the first at anything that says quite a lot because not only are you prepared, but
you have the personnel that are willing to actually put in the work,” said Col. Katrina Lloyd, state surgeon of the LANG. “We train the way we fight, and for some of our medics this was their first time to actually put their hands on live tissue. That’s important for our medics because we want them to know what to expect before being in that situation of having to work on a fellow service member because in those situations, a medic’s reaction is everything.”
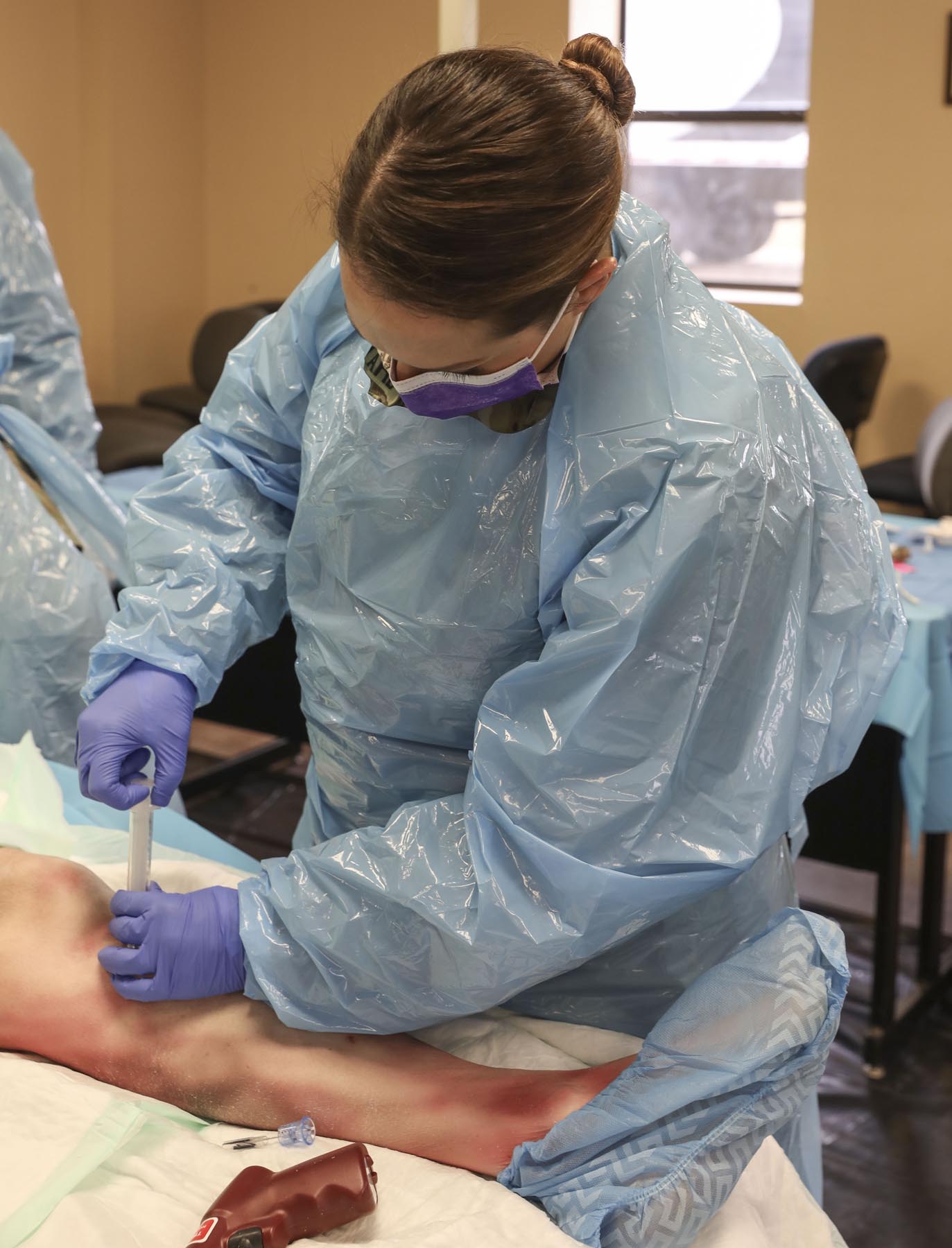
During the lab, medics were able to use the same equipment they use on missions on actual cadaveric tissue, and to learn how the tissue actually feels when conducting medical procedures. Being able to practice these procedures allowed medics to build confidence in their abilities and equipment.
“This training is important for medics because it allows you to see the same anatomy that you’re going to be working on,” said Air Force Staff Sgt. Mitchell Kraemer, a paramedic at Barksdale Air Force Base in Shreveport. “It just builds confidence by allowing medics to do a procedure that may seem scary in the field, especially if it’s the first time you’re doing it, on a human where the situation can be life or death.”
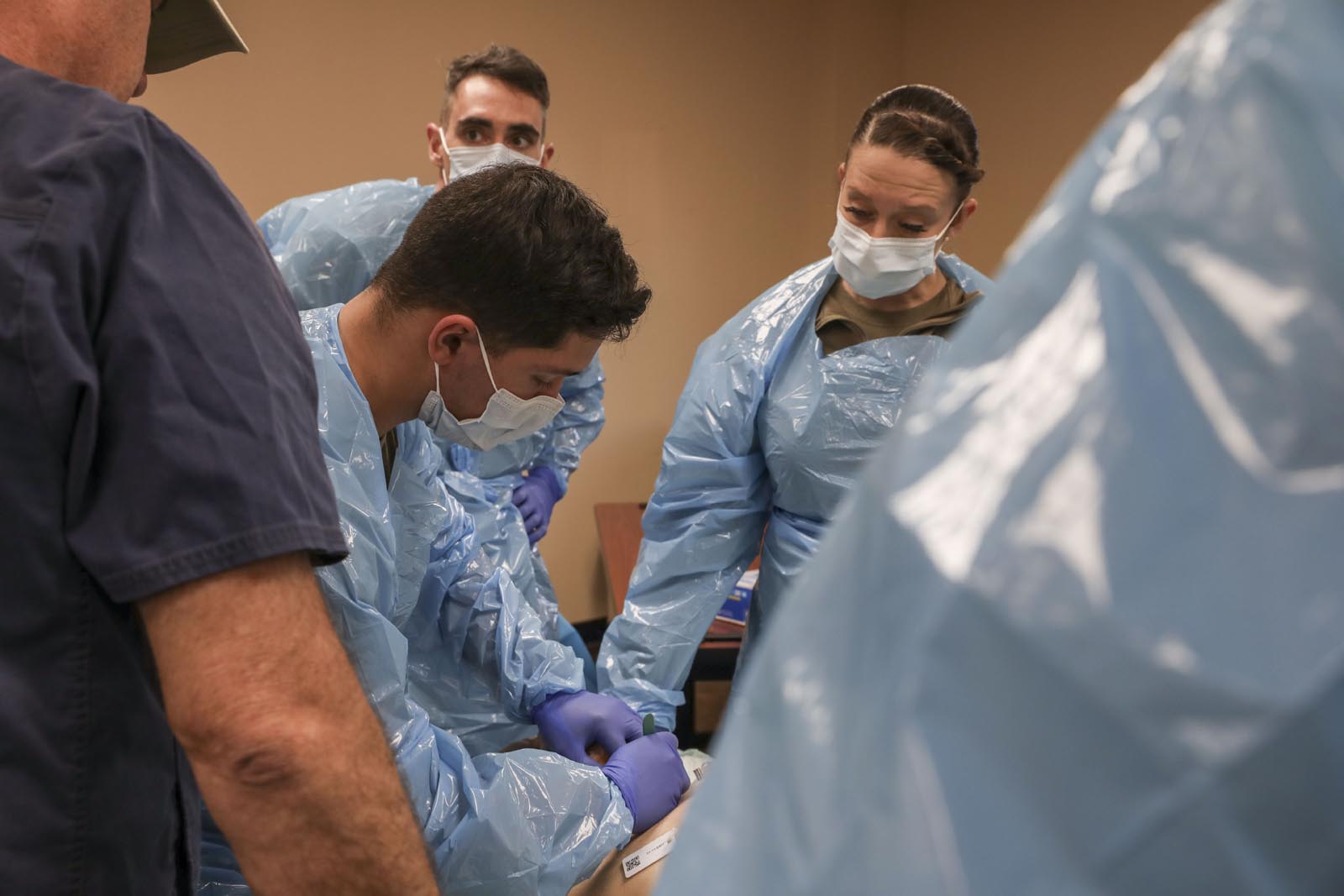
For other medics going through the training, working on the cadaveric tissue humbled them and reminded them of the humanity in the medical world.
“Sometimes we forget the human aspect of what we do because we are so used to working on or with training models, and this training just really humbled me knowing that the tissue I’d be training on once meant everything to somebody,” said New Iberia native, Spc. Kevin Sun, a medic with the Louisiana Medical Detachment. “As a National Guard medic we work a lot with the civilian populace, and we know these people. We went to high school with them or we go to church with them, and it just really brings it full circle for me realizing how important it is to get these interventions right the first time so that we can ensure the patient gets back to their loved ones.”
While working on the cadaveric tissue, Teleflex instructors walked medics through the MARCH (massive hemorrhage, airway, respirations, circulation and hypothermia) algorithm and explained multiple ways to use their standard equipment.
“What I try to do when I’m holding the class is explain to them that I’m not teaching because we both do

the same job. You’re a 68W and I’m a medic; we do the same job. So I tell people we’re having more of a conversation,” said Cruz Hernandez, an instructor with Teleflex and medic at Brooke Army Medical Center in San Antonio, Texas. “What we try to do is give medics as many tools to put in the tool box. You will never hear me say ‘this is the best way to do it’. No, the best way to do it is the way that makes you comfortable and the way that you’re most confident.”
Cadavers are provided through the Genesis Legacy Program, a whole-body donor program at MERI in Memphis, at no cost to families. The donated cadavers are within days of passing and not embalmed. After being donated, they are screened and tested for contagious diseases before they are released for training and education.
“We’ll do all of our education that we do here, but that may not be the end of the road for the cadavers. The cadavers may go to other places all over the country for other educational purposes,” said Kelli Thomas, the director of anesthesia and emergency medical clinical affairs at Teleflex Medical Equipment. “Once the full usefulness of the cadaver for educational purposes is exhausted they’ll go back to the MERI. MERI will cremate the remains and present the remains to the family along with a letter of gratitude thanking them for the donation and letting the family know where the cadaver went, how many procedures were performed, what kind of procedures and how many people had the opportunity to learn.”
Lloyd said she plans to hold more cadaver training labs in the future and build on the course.
“I think for the first training it was a great experience, and the medics I talked to really enjoyed it. They gained a lot from the experience, and they want to do it again,” said Lloyd.